The Hidden Cost of Getting Paid: A Hospital CFO's Guide to Medical Receivables Financing
You have already earned the money. You rendered the care, submitted the claim, and now you wait — 30 days, 90 days, sometimes longer — while payers process their paperwork and your payroll clock keeps ticking. In the meantime, you need capital. The question is: how much will it cost you to access what is already yours?
The answer depends almost entirely on which financing vehicle you choose. And for most hospitals, the choice has been made by default rather than strategy — with consequences that compound quietly into margin erosion, staff shortages, and a perpetual sense of financial fragility.
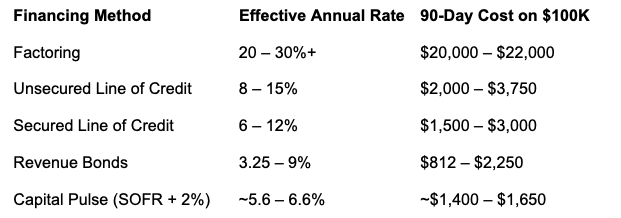
Let's examine the four traditional options, run the real numbers on a $100,000 claims portfolio, and make the case for a fifth approach that changes the calculus entirely.
The Paradox at the Heart of Hospital Finance
Hospitals operate inside a structural contradiction. They deliver services today and receive payment months from now, yet their expenses — labor, supplies, utilities, debt service — arrive on schedule regardless. The result is a chronic cash flow gap that has nothing to do with the quality of care delivered or the creditworthiness of the third-party payer.
Private and government insurers are, in fact, among the most reliable obligors in the financial system. Medicare and insurance will pay. The only question is when and exactly how much.
Traditional financing has never adequately grappled with this distinction. Instead, it has treated the hospital itself as the credit risk — and priced accordingly. The consequences fall hardest on the facilities least equipped to absorb them: safety-net hospitals, rural critical access centers, and community providers serving the populations that need them most.
Option One — Factoring: Fast Cash, Brutal Cost
Factoring is the oldest solution and, in many ways, the most honest about what it is: a transaction in which speed, in an opaque environment, is purchased at a steep discount.
A factoring company buys your outstanding claims for immediate cash — typically advancing 70 to 85 cents on the dollar, with fees that translate to effective annual rates ranging from 15% to well over 30%.
On a $100,000 claims portfolio: After a 20% discount and associated fees, you might net $78,000 — $80,000. The factor collects the full $100,000 when claims pay. Your cost of capital for the privilege of receiving your own earned revenue quickly: $20,000 to $22,000.
Why so expensive? Because traditional factors cannot accurately assess the true value of medical claims. Lacking analytical tools to distinguish a high-likelihood-to-pay Medicare claim from a contested commercial one, they apply a blunt discount to everything. Their margin isn't profit — it's insurance against their own uncertainty.
Every dollar paid to a factor is a dollar that never reaches staffing, equipment, or patient programs. It is margin erosion dressed as financing.
Option Two — Unsecured Lines of Credit: The Balance Sheet Penalty
The conventional bank line of credit sounds more respectable than factoring — and it is, marginally, in certain circumstances. But it carries its own structural flaw.
Traditional lenders evaluate the hospital's overall financial health: credit history, balance sheet strength, operating margins. Outstanding medical claims — even those owed by the federal government — are treated as opaque receivables with unpredictable timelines. They are assigned little or no collateral value.
The result: the hospital borrows against its own creditworthiness rather than against the quality of its assets. For many community and safety-net hospitals, that means accessing credit at rates between 8% and 15% — near-emergency pricing, applied to routine operational needs.
On a $100,000 claims portfolio: Carrying that balance for 90 days at 15% annualized costs approximately $3,750 in interest. Stretch the reimbursement cycle to 120 days and that figure rises to $5,000 — before fees, maintenance costs, or covenant compliance.
Rural hospitals and independent clinics are disproportionately penalized by this model. Their balance sheets are thinner not because they are poorly managed, but because they operate in markets with fewer profitable service lines and higher proportions of government-insured patients. The financing system punishes them for serving the communities that need them most.
Option Three — Secured Lines of Credit: Better Collateral, Better Rates
Secured lines of credit improve on the unsecured model by giving lenders something tangible to price against. Rather than evaluating the hospital's overall creditworthiness, the lender takes a security interest in hard assets — real property, buildings, major medical equipment, and other capital holdings. With collateral in hand, lenders can price debt more favorably.
On a $100,000 claims portfolio: Secured lending against physical assets typically prices at 6% to 12% annualized — a meaningful improvement over unsecured credit lines. The 90-day carrying cost on this portfolio runs approximately $2,000 — $3,000.
The limitation is structural. Hard assets are finite and illiquid. A hospital can only encumber its MRI suite once. And the collateral being pledged — buildings, equipment — has no logical relationship to the underlying problem, which is a timing gap between rendered services and received payment. The hospital is pledging what it owns to cover what it is owed, a mismatch that becomes increasingly strained as capital needs grow.
For facilities with strong physical asset bases, this could be a reasonable option. But it offers no path to scale, and it does nothing to address the fundamental flaw in how medical receivables are valued and financed.
Option Four — Revenue Bonds: The Prestige Problem
Revenue bonds allow hospitals — typically through a municipal or governmental authority — to access capital markets directly, bypassing conventional lenders. At their best, they offer long-term capital at relatively favorable rates.
The problem is access. Bond markets rate the institution. Investment-grade ratings flow to large academic medical centers, well-capitalized health systems, and established regional networks. Safety-net hospitals, community providers, and newer facilities face higher rates, more restrictive covenants, or outright exclusion from the market.
On a $100,000 claims portfolio: For institutions that can access bond financing, effective borrowing costs typically run 3.25% to 9% annualized — meaningfully better than unsecured credit lines, but still pricing the hospital's risk rather than the payer's.
The deeper problem is structural: the bond market is not designed for short-term working capital needs. It is a capital formation tool, not a cash flow management tool. Using it to bridge a 90-day reimbursement cycle is like using a freight train to run a local delivery route. The infrastructure doesn't fit the problem. And for the majority of community hospitals, the market isn't even available — rating agencies and bond buyers have already made that decision for them.
Option Five — Capital Pulse: Reimbursement at the Speed of the Claim
Capital Pulse represents a new, fifth category — and a fundamentally different one. Where the previous four options all price risk against the hospital's own profile (its creditworthiness, its balance sheet, its physical assets), Capital Pulse introduces something none of them have: the ability to accurately value the claims themselves.
The mechanism begins with the Healthcare Claims Scoring System (HCSS): a predictive model that predicts denials and evaluates claims with accuracy approaching 98%, assigning each claim a probability of payment, an expected timeline, and an expected value. This transforms outstanding receivables from uncertain IOUs into precisely valued, highly bankable collateral.
Because the collateral is now transparent and reliable, Capital Pulse can price financing against what it actually is: a near-certain obligation of some of the most creditworthy payers in existence. Commercial payers will pay. The federal government does not default on Medicare claims. State Medicaid programs do not vanish.
The result is financing priced at SOFR plus 200 - 350 basis points — currently in the range of 5.6% to 6.6% annualized, representing the lowest cost of capital available in the healthcare receivables market. Same-day reimbursement on qualified claims is available, eliminating the reimbursement lag entirely.
On a $100,000 claims portfolio: The 90-day carrying cost at SOFR + 2% is approximately $1,575 — $1,625. Compare that to:
The difference between factoring and Capital Pulse on a single $100,000 portfolio is more than $18,000. Across a hospital with $10 million in annual receivables, that gap compounds into a transformative financial advantage — capital redirected from financing costs back into care delivery.
The Choice Ahead
The healthcare financing system was built around a fundamental misreading of risk. Hospitals have been paying a premium — sometimes an extraordinary one — for a complexity that was never really their fault. The extended reimbursement cycle is a feature of government payment architecture, not a reflection of provider creditworthiness.
The best financing isn't traditional debt. It is gaining immediate access to the capital a hospital has already earned — priced fairly, structured intelligently, and available when a qualified claim is submitted.
Capital Pulse exists to make that possible. The money is already there. The only question is how much it costs you to reach it.
To learn more about how Capital Pulse's AI-powered claims valuation can support your facility's financial independence, visit capitalpulse.com or contact our team.